Scarlet fever: symptoms, treatment and everything else you need to know
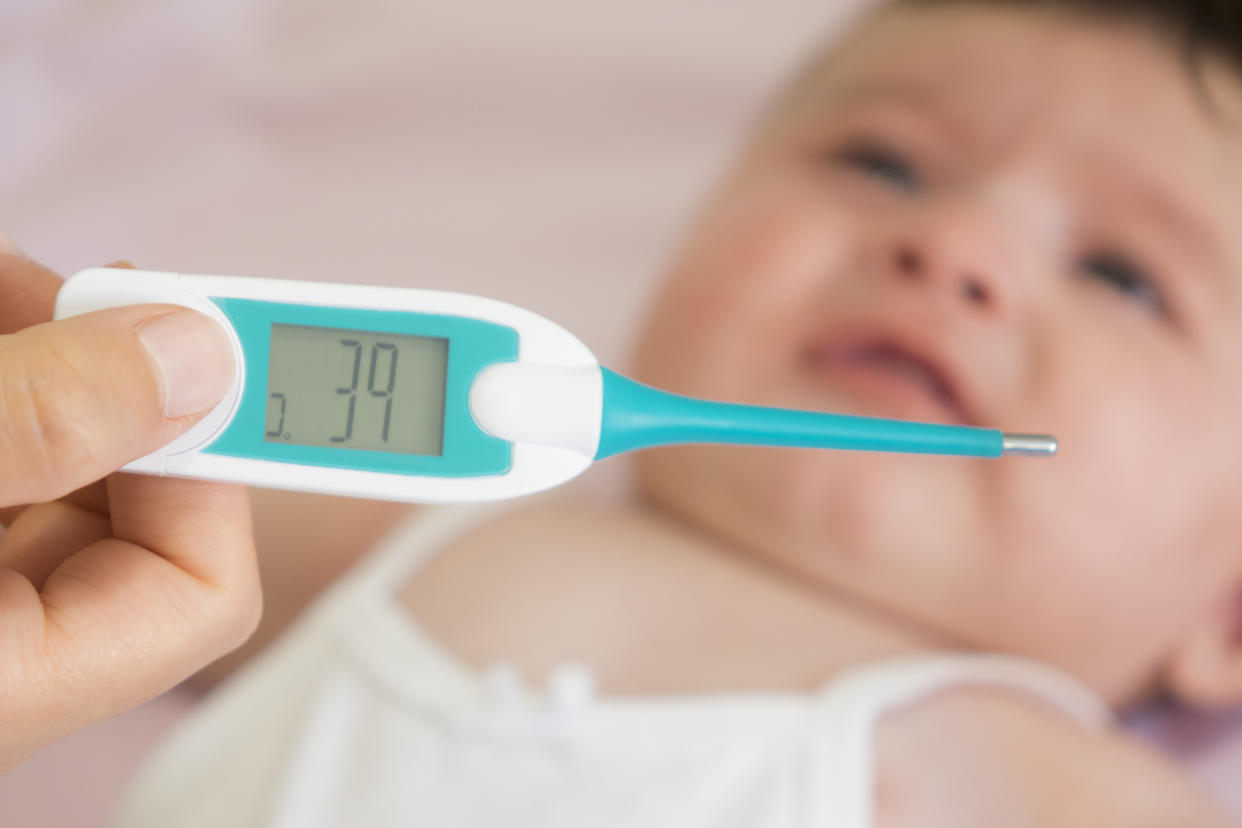
Public Health England is urging people to be aware of scarlet fever symptoms as we “move into the peak season”.
The contagious bacterial infection tends to strike during the cold winter months.
Read more: Scientists zoom in on bug behind Strep throat and scarlet fever
Once considered a disease of the 19th century, when thousands succumbed to its life-threatening complications, it has been on the rise since 2014.
Although “much less serious” than two hundred years ago, between 15,000 and 30,000 people in England still suffer the unpleasant symptoms every year.
Scarlet fever - as we move into the peak season, make sure you're aware of the symptoms:
🤒 High temperature
😫 Sore throat and swollen neck glands
👅 Distinctive rash and tongue coating
Find out more: https://t.co/AQGYpITMsQ— Public Health England (@PHE_uk) February 20, 2020
What are the symptoms of scarlet fever?
Public Health England told its 219,400 followers to look out for a “high temperature”, “sore throat and swollen neck glands”, and “distinctive rash and tongue coating”.
According to the NHS, symptoms are generally flu-like initially.
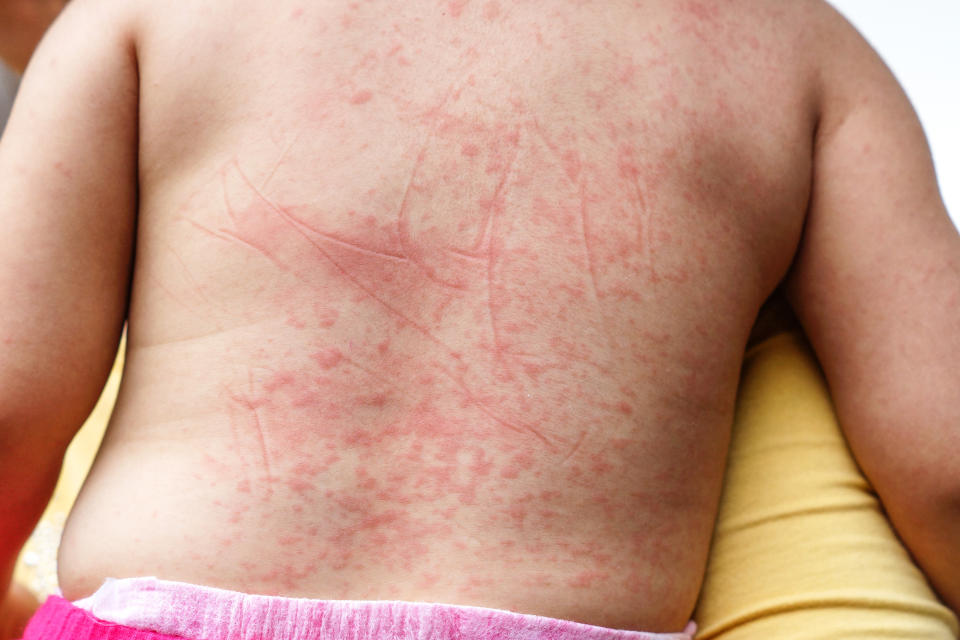
The tell-tale rash appears a few days later, feeling like sandpaper.
This generally starts on the chest and abdomen, before spreading.
On pale skin, it looks pink or red. On darker tones, the rash can be hard to spot, but still has a rough texture.
The rash does not appear on the face, however, cheeks can look flushed. This may look like sunburn on darker tones.
Read more: Father in critical condition after developing Strep infection
Once the rash has faded, some develop peeling on their fingertips, toes and groin, according to Public Health England.
Patients also suffer a “strawberry tongue”, named because of the white coating that peels, leaving it red and swollen.
Some just generally feel unwell and fatigued.
Adults and children develop the same symptoms, however, scarlet fever is “mainly a childhood disease”.
Most patients are between two and eight years old, with four-year-olds being statistically most at risk. Overall, around 90% of cases are in children under 10.
What complications can arise with scarlet fever?
Scarlet fever is rarely serious these days, however, patients should see their GP if they develop any warning signs.
If after seeing a GP the symptoms fail to clear up in a week, the NHS stresses you should arrange another appointment. This is particularly important if a child has recently had chickenpox.
Feeling ill a few weeks after “beating” scarlet fever can be a sign of rheumatic fever.
This “very rare complication” can come about after any bacterial throat infection, causing painful joints and heart problems.
Other complications can include pneumonia.
Read more: Mumps hits decade high in England
This occurs when the alveoli (air sacs) in the lungs become inflamed and filled with pus or fluid in response to an infection.
In severe cases, it can be fatal.
Other issues can include an ear infection, throat abscess - pus-filled pocket, and sinusitis - inflammation of the sinuses.
Arthritis, meningitis - infection of the membranes that surround the brain and spinal cord, and septicaemia - blood poisoning, can also occur.
On “rare occasions”, late stages of infection can affect the bones, joints, liver, kidneys and heart.
All the above are rare thanks to antibiotics preventing and treating the infection.
How does scarlet fever spread?
Scarlet fever is very infectious, spreading via the mucus and saliva of infected people.
Your GP may therefore suggest a phone consultation rather than have you come into the surgery.
Patients can avoid spreading the infection by washing their hands frequently with soap and warm water.
They should also sneeze and cough into a tissue, which is then promptly thrown away.
To ward off infection, do not share cutlery, cups, towels, clothes, bedding or baths.
Note there is no vaccine that protects against scarlet fever.
How is scarlet fever treated?
Scarlet fever is caused by the bacteria Streptococcus pyogenes, or group A streptococcus, which also cause impetigo.
These tend to respond to antibiotics, which aid recovery, reduce the risk of pneumonia and ward off spreading of the infection.
Most scarlet fever cases clear up in around week, providing it is treated.
Patients are infectious up to seven days before symptoms start until 24 hours after taking the first antibiotic tablet.
Those who do not take the medication can be infectious for between two and three weeks after symptoms appear.
Children should stay off school for 24 hours after starting antibiotics or until the fever is gone if the infection is not treated for whatever reason.
Drinking cool fluids, taking painkillers to combat fever and using calamine lotion or antihistamine tablets for itching can ease symptoms.
Soft throats may also make eating more comfortable if you have a sore throat.



