Psoriasis sufferer, 24, gets asked if she is burnt or contagious

A psoriasis sufferer has revealed how she gets confused for a burns victim and parents move their children away in case she is contagious.
Michelle Mandere developed a small spot on her arm when she was just seven years old.
After dismissing it as nothing to worry about, the spot soon spread into patches that covered her entire body, including her face.
READ MORE: Kim Kardashian details her 'painful and scary' struggles with psoriasis
Now 24, Miss Mandere endures skin that is so tighten it cracks and bleeds, leaving her in almost constant pain.
For years the support worker would cover her skin, embarrassed by what others would think.
Having made peace with the condition, Miss Mandere refuses to let it hold her back, telling other sufferers “you can do anything”.

Miss Mandere was living in her native Zimbabwe when she developed the itchy spot out of nowhere.
Speaking this Psoriasis Awareness Week, she told Yahoo UK: “No one paid it much mind but it gradually started to spread to another place and became more itchy.
“The spot turned into a patch and the patch would spread.”
After trying various herbal remedies, Miss Mandere’s mother eventually took her to a GP around a year later.
“Even when I went to the doctor, nobody knew what was wrong with me,” she said.
After another year of back and forth, Miss Mandere was diagnosed with psoriasis in 2004, just before she moved to Nottingham.
The support worker has endured almost daily discomfort ever since.
READ MORE: Smoking, excess alcohol, stress and anxiety can trigger psoriasis
“Your skin is constantly dry,” she said. “It feels like your skin is tightening up, that’s when the pain comes in.
“When you move you get cracks and then it bleeds.
“If you moisturise, it’s soft for maybe an hour, and then it’s dry and aching again.”
As well as coping with the symptoms, Miss Mandere is also forced to endure cruel comments and stares from strangers.
“People stare at me,” she said.
“I’ve had people ask if I got burnt when I was younger or if I’m contagious and if it’s safe for me to be around their children.
“Children on the bus will ask, ‘mummy why is her face like that?’”
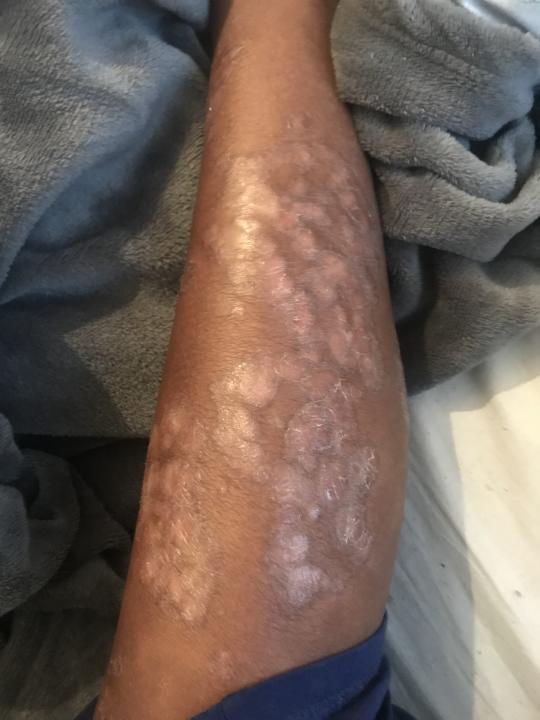
Miss Mandere, who works closely with the Psoriasis Association, takes the immune-suppressing drug methotrexate.
Psoriasis comes about when skin cell production speeds up, according to the NHS.
Skin cells are normally replaced every three-to-four weeks, however, psoriasis accelerates this to between three and seven days.
This is thought to be due to the immune system mistakenly attacking healthy skin cells.
Methotrexate binds to and inhibits an enzyme involved in the rapid growth of skin cells, slowing it down, according the the National Psoriasis Foundation.
Although effective, the drug also suppresses a patient’s immune system, leaving them more vulnerable to infections.
Miss Mandere, who is training to be a mental health nurse, was forced to come off the medication in March to have a chickenpox vaccine.
“Part of the course is making sure all your vaccinations are up-to-date for when you go on hospital placements,” she said.
READ MORE: 'It broke my confidence': How this woman with psoriasis learned to love her 'cheetah spots'
Miss Mandere is now waiting for her second dose of the jab.
Meanwhile, being off methotrexate has caused her skin to flare up.
Although reasonably effective, the drug is by no means a “cure”.
“It kept my skin clear but it would reach a plateau where my skin would get used to it,” Miss Mandere said.
“Then I would increase the dose, then my skin would get used to it again.”
Miss Mandere also had to contend with the mouth ulcers and nausea that can come from taking methotrexate.
In an attempt to clear up her skin “naturally”, she recently cut out dairy, which has helped somewhat.
“My skin has stabilised,” Miss Mandere said. “It’s not getting worse or better.”
The NHS recommends patients learn, and avoid, their triggers. These can include excessive alcohol, smoking and stress.
Despite all she has endured, Miss Mandere refuses to let her psoriasis hold her back.
READ MORE: Are you suffering from psoriasis? Symptoms, triggers and how to treat
“A few years ago I would make sure my outfit on a night out was covered, she said. “I never wore dresses.
“I reached a stage where I thought, ‘why should I do it just to make other people more comfortable? I’ll never see these people again, why does it matter?’”
While she tries hard to stay positive, Miss Mandere admits her condition can get her down.
“I don’t mind it on my body because I can wear polo necks and long sleeves,” she said.
“But when it’s on my face I’m very paranoid. I feel like everyone is looking at me.”
Miss Mandere is speaking out to help make other psoriasis sufferers feel less alone.
“You are an individual by yourself,’ she said.
“Yes you have psoriasis but it’s not something that defines you. You can do everything that everyone else does.”
She also hopes to help people without the condition be more understanding.
“Be kind to people,” she said. “You don’t know what they’re going through or their mental state.”
Psoriasis affects around 2% of people in the UK, NHS statistics show.
In the US, more than eight million suffer, according to the National Psoriasis Foundation.


