Mother, 42, reveals car crash left her battling an antibiotic-resistant infection

A mother-of-two has revealed how a car crash left her battling an antibiotic-resistant infection.
Vanessa Carter, 42, from Johannesburg, South Africa, was a passenger when the vehicle spun out of control in 2004, hitting a concrete wall.
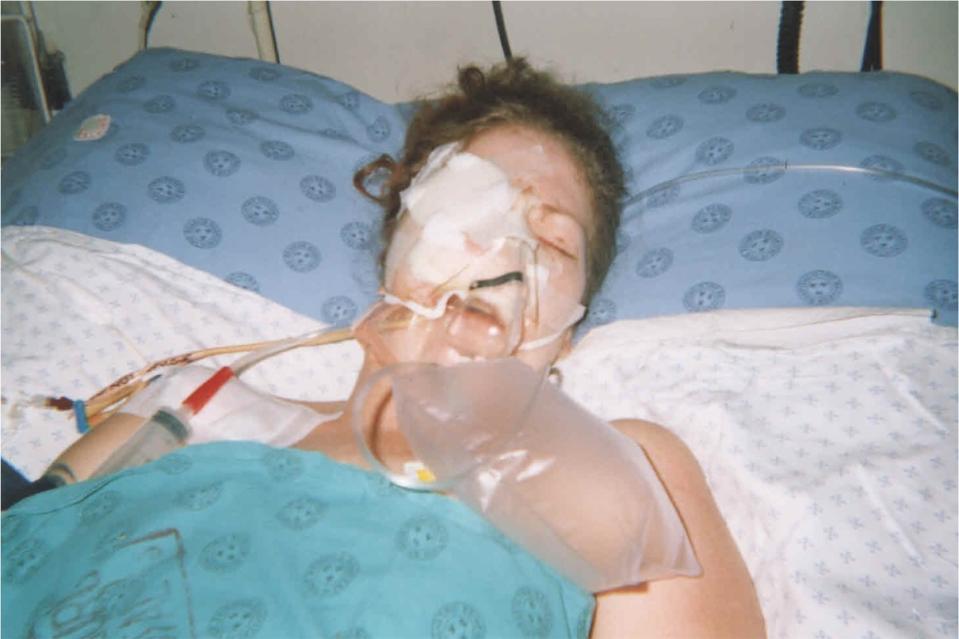
Carter had to be resuscitated at the scene, with the collision causing internal bleeding, broken bones and even the loss of her right eye.
As different doctors worked to treat her injuries over the following years, Carter had a prosthetic implanted in her right cheek in 2010, which became infected.
Despite pus coming out of her skin “continuously”, medics could not agree whether to remove the implant and continued to prescribe different courses of antibiotics.
Read more: AI helps scientists find antibiotic-like drug that kills superbug in mice
A cosmetic surgeon eventually insisted she have the prosthetic taken out, with test results revealing it was coated with the “superbug” methicillin-resistant Staphylococcus aureus (MRSA).
MRSA is a type of bacteria that are immune to many commonly-used antibiotics, making them harder to treat. It lives harmlessly on the skin of around one in 30 people, but can enter the body via a wound, feeding tube or catheter.
While Carter continues to live with her injuries, the mother-of-two is speaking out to raise awareness of antibiotic-resistant infections and why patients should take every course of drugs as prescribed.

Antibiotic resistance is causing a growing number of bacteria to no longer respond to once life-saving drugs.
The World Health Organization calls it “one of the biggest threats to global health”, with pneumonia, tuberculosis and gonorrhoea becoming increasingly difficult to treat.
Over the years, many doctors have mistakenly doled out antibiotics to treat viruses, despite the drugs only being effective against bacteria.
Antibiotics are unlike many other drugs in that the more they are used, the less effective they become.
Read more: Bust drug companies stunt antibiotic discoveries
In 2015, antibiotic use in England alone had increased by 6.5% over the past four years. In the US, at least 30% of antibiotics are said to be “unnecessary”.
More than 2.8 million antibiotic-resistant infections arise every year in the US alone, killing over 35,000 people.
MRSA specifically results in more deaths in the US every year than HIV, Aids, Parkinson’s, emphysema and murder combined.
‘I woke up in hospital five days later’
Carter remembers little of the night of the collision, but occasionally has flashbacks to getting dressed for dinner.
On the way home, a car is said to have overtaken the vehicle Carter was a passenger in, causing the driver to swerve.
Read more: Runny nose sign you don’t need antibiotics
“We caught the curb,” she told Yahoo UK. “The car spun and hit a concrete wall.
“I had my seatbelt on but was leaning forward. As the car spun, I got locked in that position.
“It was an old car without airbags.
“Then I woke up in hospital five days later on morphine.”
Carter endured multiple injuries, including a fractured pelvis and post-traumatic amnesia.
Then 25, she did not have private healthcare insurance and relied on medical aid.
Describing South Africa’s healthcare system as “very underfunded”, Carter claims she had to “figure out what doctor to see first”, with her treatment involving ophthalmologists, facial surgeons and neurologists, to name a few medics.
Carter had her first facial prosthetic two years after the accident, however, it was the implant fitted in 2010 that became infected with MRSA.
She puts this down to a delay in treatment, as well as different medics overseeing her care, each prescribing their own course of antibiotics.
“Doctors all have their own specialities, but they’re all very similar,” said Carter, who features in the report AMR [antimicrobial resistance] Voices.
“I had to find these sub-specialities and get them to work together.
“The [different] doctors were not talking to each other.”
Read more: Honey should be go-to for easing coughs
Carter is said to have lived with MRSA for around a year.
“The antibiotics weren’t working,” she said. “The infection was getting worse and worse.
“There was pus coming out of my face continuously.”
Carter claims the bacterial infection was “eating her skin”, with the itchiness feeling like “ants on her face”.
After years’ worth of operations, Carter had “built up a very good friendship with her cosmetic surgeon”.
“I was going for a sinus drainage and he said, ‘I’m going to be in the theatre next door, if I come in and see the infection is on the implant I’m taking it out’,” said Carter.
“I woke up and he had taken it out.
“I knew he’d sent it for testing. The pathologist said it was MRSA.”
Although Carter has endured no lasting complications from the infection itself, the surgeon has warned the bacteria could have entered her bloodstream, triggering life-threatening septicaemia.
Now understanding the seriousness of antibiotic-resistant infections, Carter worries the scale of the issue is “not common knowledge”.
“Doctors take it for granted that if they give a patient an antibiotic they know what to do with it,” she said.
“If you don’t know, you don’t take your antibiotic seriously.
“I was stopping my antibiotics halfway thinking ‘they’re not working’, but that makes it worse.”
Carter believes the “public education messages to tackle COVID-19 [the disease caused by the coronavirus] are a good foundation to build on and raise awareness of antibiotic resistance”.
Daniel Berman from Nesta Challenges – the company behind the AMR report – added: “Life-threatening resistance to antibiotics is not some dystopian fiction.
“The all hands on deck battle against COVID-19 needs to be replicated to address antimicrobial resistance.
“This includes better strategies for developing new antibiotics; new and innovative treatment techniques; continued improvement in stewardship, infection control and hygiene; and accelerated investment towards the development of new rapid diagnostics.”
How to help prevent antibiotic resistance
Random mutations take place within bacteria at a rapid rate.
Exposure to an antibiotic “selects” for mutations that protect the bug from destruction. Bacteria can pass this genetic advantage to future generations or “horizontally” to other bugs.
Many patients fail to take antibiotics as prescribed, coming off them when they feel better.
This could mean they stop treatment before the bacteria have been eradicated from the body, giving the bugs a better chance of developing resistance.
Antibiotics can save lives and should always be taken if prescribed, however, patients can help stem resistance.
Always take the drug as prescribed, never sharing or skipping doses.
The NHS stresses multiple antibiotics should be equally spaced throughout the day and taken at the same times every day to help “maintain a constant level of medicine in your body”.
Return any unused antibiotics to a pharmacy for safe disposal. Do not throw them out, flush them away or store for future use.
Antibiotics are ineffective against viruses. Patients should therefore not pressurise their GP to prescribe the drugs if they have a cold or flu.
Many bacterial infections also have vaccines, like diphtheria. Keeping up-to-date on jabs could prevent the infection taking hold in the first place.
Infections can also be stemmed via good hand hygiene, staying home when ill and coughing into your elbow.
Watch: Antibiotic resistance and what can be done about it


