AI helps scientists find a new ‘antibiotic’ that kills superbug in mice
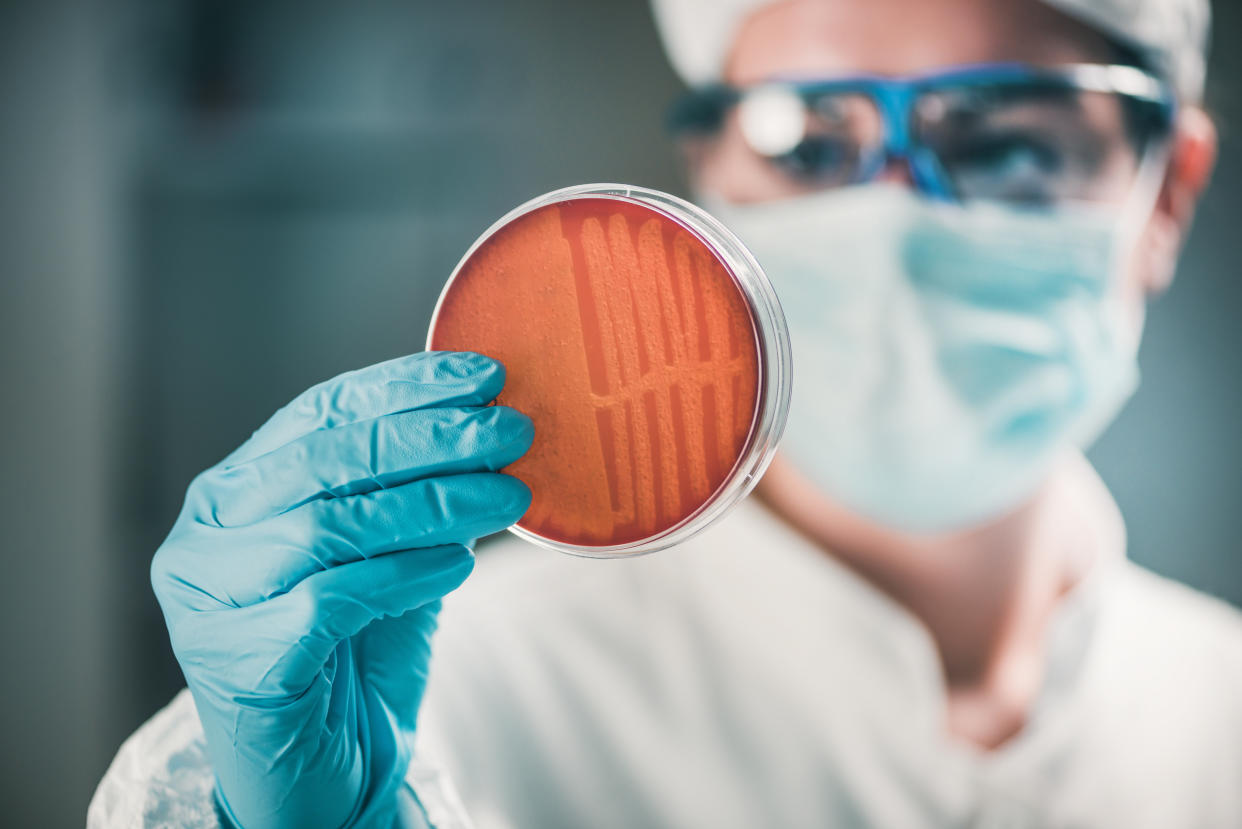
Artificial intelligence (AI) helped scientists discover an antibiotic-like molecule that could target “superbugs”.
Antibiotic resistance is causing a growing number of bacteria to no longer respond to once life-saving drugs.
Read more: This is what people think is the biggest threat to global health
The World Health Organization calls it “one of the biggest threats to global health”, with pneumonia, tuberculosis and gonorrhoea becoming increasingly difficult to treat.
This has led to the rise in superbugs, like MRSA and Clostridium difficile (C.diff).
Antibiotics are naturally produced by soil bacteria and fungi.
Rather than rummaging through dirt, a team from the Massachusetts Institute of Technology used machine learning to sift through a “drug-repurposing database”.
A “deep neural network” looked at more than 107 million molecules to predict which may have “antibacterial activity”.
They identified a molecule called halicin, initially suggested as a diabetes drug.
When tested on mice, it “killed off” C.diff.
C.diff can infect the bowel, causing diarrhoea.
It usually affects those who have taken antibiotics, which interfere with the balance of “good bacteria” in the gut, causing “bad” pathogens to multiply.
Read more: Antibiotic resistance 'could wipe out humanity before climate change’
C.diff is “known to be resistant to multiple antibiotics commonly used in the treatment of bacterial infections”.
Although usually harmless, the infection kills around 29,000 people a year in the US alone.
Results, published in the journal Cell, reveal Halicin was also effective against the bacteria Acinetobacter baumannii in mice.
A.baumannii can trigger pneumonia or infection of the blood or urinary tract, killing around 700 people a year in the US.
Halicin is structurally different from antibiotics, but effective nevertheless.
“We’re finding leads among chemical structures that in the past we wouldn’t have even hallucinated could be an antibiotic,” Professor Nigam Shah from Stanford University told STAT news.
What causes antibiotic resistance?
Over the years, many doctors have mistakenly doled out antibiotics to people battling viruses.
“Antibiotics only work against bacteria, through actions such as disrupting their cell wall to kill them or suppressing their division and growth while your own immune system fights them off,” Dr Sarah Brewer, medical director of Healthspan, previously told Yahoo UK.
“Viruses have a very different biology and do not respond to these actions.”
Antibiotics are unlike many other drugs in that the more they are used, the less effective they become.
In 2015, antibiotic use in England alone had increased by 6.5% over the past four years.
At least 30% of antibiotics prescribed in the US are “unnecessary”.
Random mutations take place within bacteria at a rapid rate.
Exposure to an antibiotic “selects” for mutations that protect the bug from destruction.
Bacteria can pass this genetic advantage to future generations or “horizontally” to other bugs.
When correctly given out for bacterial infections, many patients fail to take antibiotics as prescribed, coming off them when they feel better.
This could mean they stop treatment before the pathogen has been eradicated from their body, giving it a better shot of developing resistance.
When will antibiotic resistance strike?
Antibiotic resistance is underway.
More than 2.8 million antibiotic-resistant infections arise every year in the US, killing over 35,000 people.
One of the most well known is MRSA, methicillin-resistant Staphylococcus auerus.
S. auerus lives harmlessly on the skin of around one in 30 people.
If it gets into the body, it can infect the blood, lungs and urinary tract.
MRSA is usually treatable via non-methicillin antibiotics.
Nevertheless, it kills more Americans every year than HIV, AIDS, Parkinson’s, emphysema and murder combined.
Read more: This microbe is spreading antibiotic resistance to other bacteria
There may come a time when bacteria stop responding to antibiotics altogether.
Bacteria are constantly mutating, with some leading to resistance and others not.
The development of new antibiotics has “essentially stalled due to economic and regulatory obstacles”, with 15 of the 18 biggest pharma companies “abandoning the antibiotic field”.
Seeing as antibiotics are used for a short time and are “curative”, they are “not as profitable as drugs that treat chronic conditions”.
Once resistance develops and the drug is ineffective, “profits prematurely curtail”.

How you can help prevent antibiotic resistance
Antibiotics can save lives and should always be taken if prescribed, but you can help stem resistance.
If you feel your doctor is too keen to suggest antibiotics, the Centers for Disease Control and Prevention recommends asking if there is another way you can combat the infection.
When antibiotics are necessary, take them as prescribed, never sharing or skipping doses.
Throw out leftover pills, rather than storing them for future use.
The US Food and Drug Administration recommends mixing leftover drugs with “something undesirable”, like coffee grounds or cat litter.
This makes it less appealing for anyone going through bins, like children or pets.
Throw the mix away in a sealed bag.
Antibiotics are ineffective against viruses. You should therefore not pressurise your GP to prescribe them if you have a cold or flu.
Many bacterial infections also have vaccines, like diphtheria.
Keeping up-to-date on your jabs could prevent the infection in the first place.



