Why are fewer people getting vaccinated?
A fall in vaccination rates is leaving many vulnerable to once “eradicated” diseases.
Some blame social media for peddling “anti-vaxx” conspiracy theories, while others claim they just don’t have time for an appointment.
Read more: Should we be concerned less children are having vaccines?
Edward Jenner, “the father of immunology”, noticed milkmaids who battled the mild cowpox virus did not develop smallpox – one of the biggest killers of the 18th century.
Similar to today’s vaccines, Jenner inserted pus from a cowpox pustule into an eight-year-old boy’s arm, leaving him “immune” to smallpox.
Fast-forward more than 200 years, vaccines prevented at least 10 million deaths worldwide between 2010 and 2015 alone.
Why are vaccination rates falling?
While the anti-vaxx movement may feel recent, “research” linking the whopping cough jab to brain damage caused uptake to plummet to around 30% in the mid-1970s.
This led to an outbreak in 1978, with 65,000 cases and 12 children dying.
A 1981 study suggested the brain damage risk was “tiny” – around one in 310,000 – yet it still took 15 years for vaccinations rates to climb back to before the scare.
“We thought the health intervention [of vaccinating] would be as normal as tooth brushing, but we’ve had some challenges,” said Dr Heidi Larson from the London School of Hygiene & Tropical Medicine.
“[Concerns are] safety, safety, safety.”
Perhaps the most famous scare story was the MMR-autism headline that hit in the late 1990s.
Former gastroenterologist Andrew Wakefield mistakenly linked the measles, mumps and rubella (MMR) jab to autism in the medical journal The Lancet.
The paper has since been retracted and Wakefield struck off.
The “data” has been called “bogus”, as well as “fatally flawed both scientifically and ethically”.
Nevertheless, it appears fears have persisted.
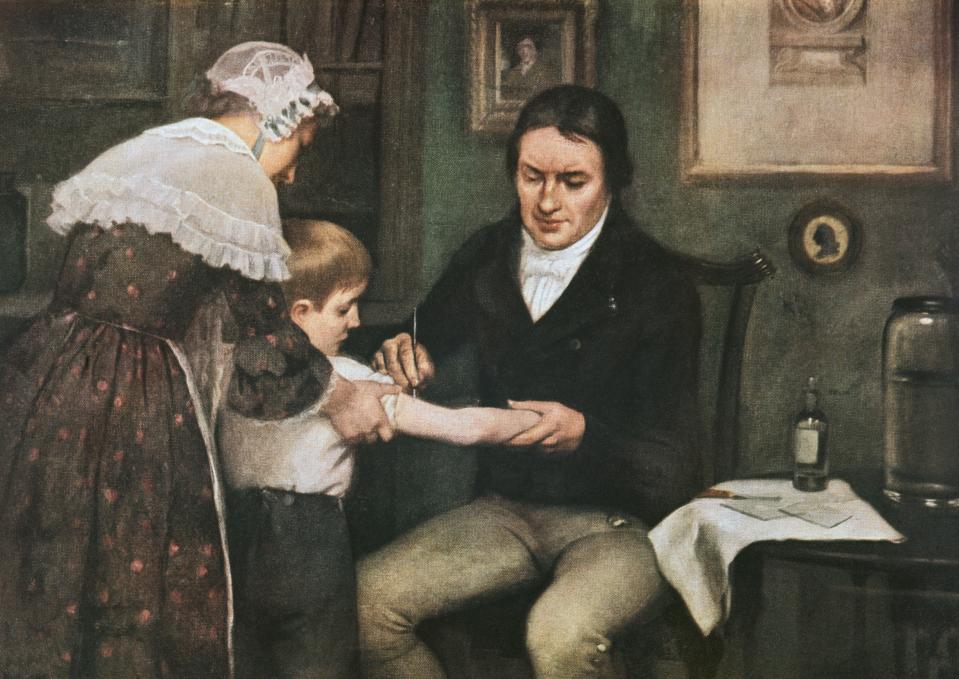
The NHS offers the MMR as part of its routine childhood immunisation schedule.
One dose is given when a child is around 12-to-13 months, followed by a booster at three years and four months.
NHS Digital data shows 94.5% of five year olds in England had been immunised with the first dose in 2018/19, down from 94.9% in 2017/18 - both below the 95% target.
An immunisation rate of 95% can ward off an outbreak due to “herd immunity”.
Herd immunity means enough of the public have been vaccinated for an infection not to be able to “take hold”.
This protects those who may be unable to get vaccinated, like cancer patients.
Read more: Coronavirus vaccine 'will not be available until mid-2020', pharma exec warns
When it comes to the second MMR dose, 86.4% of five-year-olds in England were immunised in 2018/19, down from 87.2% the year before.
In 2017, the World Health Organization declared the UK had “eliminated measles” based on 2014-to-16 data.
This was reversed when 991 confirmed cases came to light in England and Wales in 2018.
Speaking at the Royal Society of Medicine, Dr Larson said: “This is a repercussion of gaps in MMR uptake.
“We thought we’d see mumps and here we are.”
Cases of mumps in England have reached a decade high.
Outbreaks in universities and colleges led to 5,042 cases in 2019, four times as many as 2018.
This is the highest cases have been since 7,662 incidences were reported across England and Wales in 2009.
While it may be tempting to blame anti-vaxxers, the situation is likely far more complex.
“Anti-vaxxers are a very small group of people but they’re very opportunistic,” said Dr Larson.
She noted global conflicts also slow immunisation programmes, while some patients just get frustrated trying to book an appointment.
“Anti-vaxxers may be the tipping point,” said Dr Larson.
The MMR’s ability to protect against mumps may also wear off over time, which could be partially responsible for the outbreak.
Read more: Alzheimer's vaccine could be trialled on humans in two years
MMR jab aside, the UK gets a “gold star” when it comes to HPV vaccinations.
Human papillomavirus (HPV) is a sexually-transmitted infection that four in five Brits catch at some point.
It is behind 99.7% of cervical-cancer cases.
NHS England offers the first jab against HPV to boys and girls aged 12-to-13. The second comes six-to-12 months later.
Since it was rolled out in 2008, 10.5 million doses had been administered in the UK by 2018.
This slashed infections of high-risk HPV strains by 86% in young women and reduced pre-cancerous cervical disease by around 71%.
Nurses often go to schools to administer these jabs, while parents have to take young children to get vaccinated.
When it comes to the MMR, Dr Mary Ramsay – head of immunisation at Public Health England – noted uptake of the second dose is markedly lower than the first.
“The decline is not in commencing vaccination but in completing courses,” she said.
Difficulty booking an appointment amidst life’s chores may be a real hinderance.
“The system tends to be inflexible,” said GP Dr Gary Marlowe.
“[You’re told] this is the clinic and these are the nurse times.”
Dr Marlowe noted patients praise simple interventions, like having toys in the waiting area or appointments available on Sundays.
The NHS has pledged to provide services at a convenient time.
With pharmacies often also offering vaccinations, ask your local branch for advice in securing jabs.



