The coronavirus chart that 'explains Boris Johnson's drastic action'

Scientists from Imperial College London have put together a chart that may explain why Boris Johnson has taken such extreme action amid the coronavirus outbreak.
On Monday, the prime minister urged Britons to avoid social contact, ditch non-essential travel and work from home, if possible.
Entire households have also been told to self-isolate for 14 days if just one member has the tell-tale fever or cough, not even venturing out to buy “food or essentials”.
While it may sound extreme, a model put together by the Imperial team suggests such measures are necessary to free up critical-care beds.

The new Covid-19 virus is thought to have emerged at a seafood and live animal market in the Chinese city Wuhan, capital of Hubei province, at the end of last year.
It has since spread internationally, with more than 185,000 confirmed cases since the outbreak was identified, according to John Hopkins University data.
Early research suggests four out of five cases are mild, with over 80,000 patients now “recovered” from the virus.
Latest coronavirus news, updates and advice
Live: Follow all the latest updates from the UK and around the world
Fact-checker: The number of Covid-19 cases in your local area
Explained: Symptoms, latest advice and how it compares to the flu
Nonetheless, the global death toll has exceeded 7,300.
Although the outbreak began in China, its cases have been plateauing since the end of February.
Europe is now the epicentre of the pandemic, with Italy alone having more than 27,900 confirmed cases and over 2,000 deaths.
More than 37,000 people have been tested in the UK, of whom 1,553 have come back positive. Fifty-five patients have died.
Why extreme measures may be necessary to combat the coronavirus
UK officials have reportedly used the Imperial team’s predictions to guide them in combatting the coronavirus.
The UK is aiming to “suppress” the outbreak, “reducing case numbers to low levels and maintaining that situation indefinitely”, rather than “mitigating” it.
Mitigation focuses on “slowing but not necessarily stopping epidemic spread” by protecting the elderly and already ill, who are most at-risk.
The suppressing approach is thought to save more lives, but reduces hopes the public will build up herd immunity.
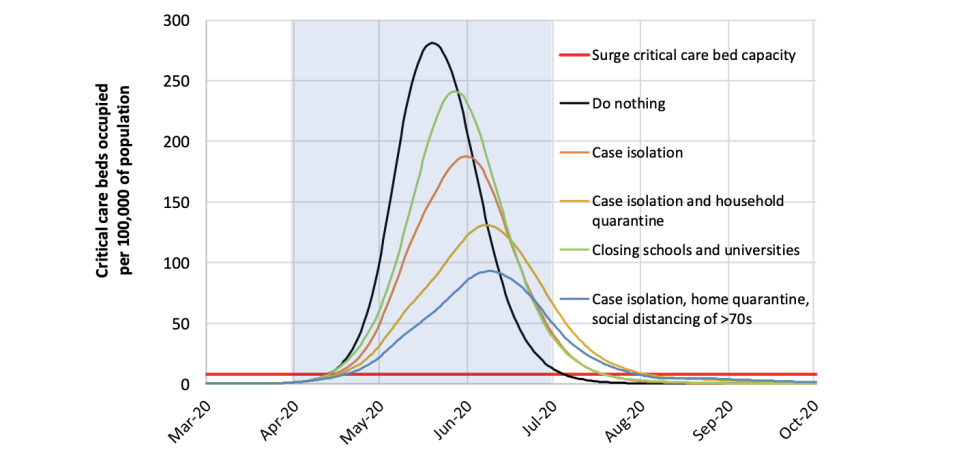
The Imperial scientists based the above chart on a simulation model “developed to support pandemic influenza planning”.
If Britons did not change their behaviour, allowing the coronavirus to spread readily in the community, the chart shows around 275 beds would be occupied for every 100,000 people in the UK come mid-May.
This could result in the critical-care bed capacity being “exceeded as early as the second week in April”, the scientists wrote.
The peak out of the outbreak could then result in a demand for beds that is “over 30 times greater than the maximum supply” in both the UK and US.
Interventions are being put in place to prevent this happening, known as “flattening the curve”.
These may help reduce case numbers and therefore deaths, with timing seemingly being everything.
“Introducing such interventions too early risks allowing transmission to return once they are lifted; it is therefore necessary to balance the timing of introduction with the scale of disruption imposed and the likely period over which the interventions can be maintained”, the scientists wrote.
The UK is yet to close schools and universities, despite such measures being implemented everywhere from Ireland to New York.
Experts have warned such closures need to be properly timed to avoid doing more harm than good.
Nonetheless, the Imperial scientists found temporarily shutting the education system would mean around 240 beds are occupied per 100,000 people, while also shifting the “peak” towards June.
The self-isolation of cases – as officials have long urged the public to do – would bring this down to around 190 beds being occupied per 100,000 people.
Case isolation combined with “household quarantine”, the latest government measure, could mean 125 beds are full in critical care per 100,000 members of the population.
This may also shift the peak of the UK’s outbreak to mid-June, when the NHS is under less strain from seasonal flu.
Combining “home quarantine” with case isolation and social distancing among the elderly could mean around 90 critical-care beds are occupied per 100,000 people, with the outbreak reaching its worst stage during the northern hemisphere’s summer.
The best approach of all would be to increase the critical care capacity.
The NHS is reportedly in talks to take up beds in private hospitals in anticipation of the situation worsening.
Although the vast majority of patients do not require hospitalisation, some develop pneumonia.
This occurs when the respiratory infection invades the air sacs in the lungs, causing them to become inflamed and filled with pus or fluid.
The lungs then struggle to draw in air, resulting in reduced oxygen in the bloodstream.
While Covid-19 has no “set” treatment, some patients are being put on a ventilator while their immune system works to fight off the infection.
Boris Johnson has told British manufacturers to scale up the production of ventilators, which the government will buy.
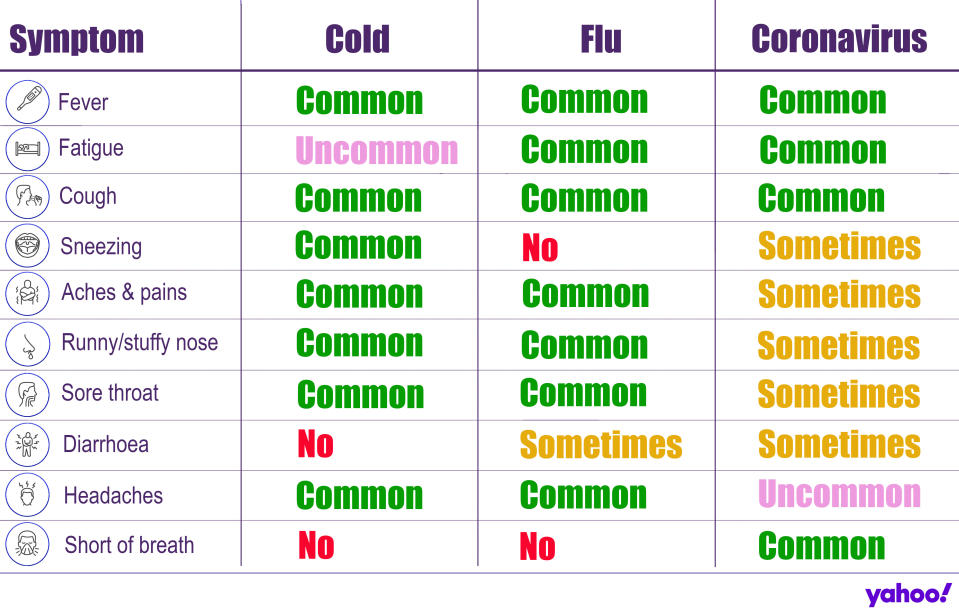
What is the coronavirus Covid-19?
The Covid-19 strain is one of seven of the coronavirus class that are known to infect humans.
Others include the common cold and severe acute respiratory syndrome (Sars), which killed 774 people during its 2002/3 outbreak.
Most of those who initially caught the Covid-19 virus worked at, or visited, the market in Wuhan.
The pathogen mainly spreads via infected droplets that have been coughed or sneezed out by a patient.
There is also evidence it may be transmitted in faeces and urine.
To ward off infection, officials urge people to wash their hands regularly and maintain social distancing.




