Death rates halved among critically-ill COVID patients in England in just three months, study suggests
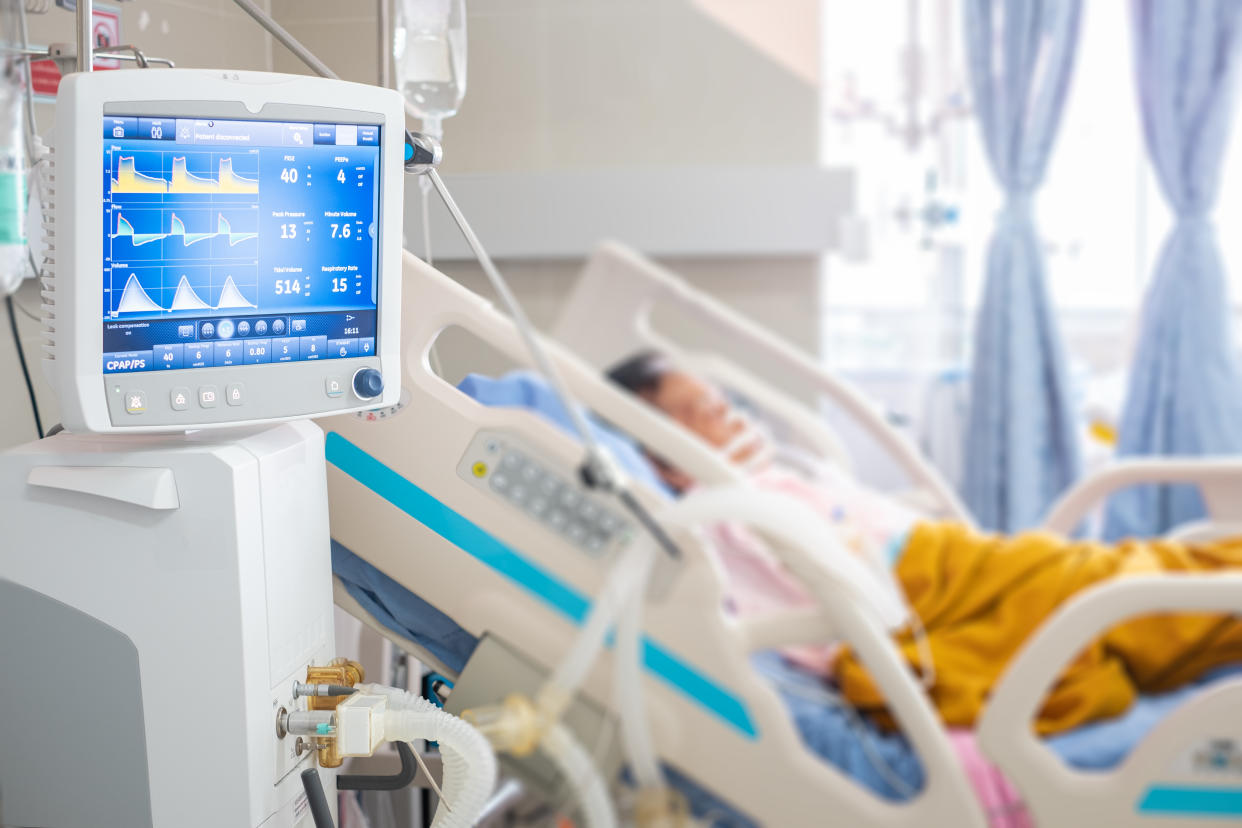
Death rates among critically-ill coronavirus patients in England have halved since their peak at the height of the outbreak, research suggests.
Scientists from the universities of Exeter and Warwick analysed more than 21,000 admissions across 108 critical care units between March and June.
Deaths peaked in late March, when just over two in five (41%) patients admitted to intensive care and a quarter (26%) in high dependency units died with coronavirus complications.
Just three months later, death rates dropped to 21% among those in intensive care and 7% among high dependency patients.
Read more: 14% of all UK coronavirus deaths linked to air pollution
With the coronavirus only identified at the end of 2019, medics have come a long way in understanding the infection over a relatively short period of time.
The virus initially had no set treatment, with critically-ill patients being offered supportive care – like ventilation – while their immune system worked to fight off the infection naturally.
Encouraging studies into low-cost steroids have since “added a further weapon in the armoury in the worldwide fight against COVID-19 [the disease caused by the coronavirus]”.

The UK is in a dreaded second coronavirus wave, with cases on the rise in almost every region.
A further 20,890 incidences were reported on 26 October, while 102 people died within 28 days of a positive test.
Read more: Harvard doctor describes mourning a loved one amid the pandemic
This case number is substantially higher than the 5,130 incidences confirmed on 8 April, the same day the government reported a record 1,073 people died with the infection.
While it may seem the UK is approaching a worse situation than its first wave, experts have stressed as many as 200,000 cases were likely occurring a day in March, with insufficient testing meaning these incidences were missed.
Watch: Can you catch coronavirus twice?
To better understand how coronavirus death rates have changed, the scientists analysed the number of adults admitted to critical care with the infection via the COVID-19 Hospitalisation in England Surveillance System (CHESS).
CHESS, which is put together by Public Health England, records the proportion of people with the coronavirus dying within 30 days of hospital admission.
“There has been a substantial improvement in survival amongst people admitted to critical care with coronavirus disease 2019 in England, with markedly higher survival rates in people admitted in May and June compared with those admitted in March and April,” concluded the scientists.
Lead author Dr John Dennis, from the University of Exeter, added: “Importantly, we controlled for factors including age, sex, ethnicity and other health conditions such as diabetes.
Read more: How to breastfeed safely during the pandemic
“This suggests the improvement in death rates in more recent months is not simply due to younger, or previously healthier, people being admitted to critical care.
“A number of factors are likely to be at play here, including improved understanding of how to manage COVID-19 amongst doctors and the introduction of effective treatments.”
In June, scientists from the University of Oxford announced the steroid dexamethasone cut the risk of death by one third in COVID patients receiving ventilation.
Three months later, a review of seven studies – co-ordinated by the World Health Organization – found dexamethasone and fellow steroids hydrocortisone and methylprednisolone reduced the risk of death by an estimated 20%.
The NHS said it would “take immediate action” to ensure patients who could benefit from steroids receive them, “adding a further weapon in the armoury in the worldwide fight against COVID-19”.
The latest study may seem encouraging, however, the scientists have stressed the public must not become blasé as we work to fight the pandemic.
“The reduction in the number of people dying from COVID-19 in hospitals is clearly a step in the right direction, but it’s important we do not become complacent as a result,” said co-author Dr Bilal Mateen, from the University of Warwick.
“It’s possible the higher death rates at the peak of the pandemic are in part because hospitals were so overcrowded at that point.
“Even at the lowest point, nearly a quarter of admissions to intensive care were still dying.
“That’s a huge number of people, and we have to do all we can to control the spread of the virus and keep hospital admissions as low as possible.”
Watch: What is long COVID?



