Bald ambition: Why I had a hair transplant at 28

It was not long after my 22nd birthday that I first spotted my dodgy hairline. Having just left university, I decided to chop away at my shoulder-length mane. It was time, I decided, to sport a close crop and embrace adulthood.
Afterwards, the bathroom mirror revealed the bleak truth. Follicles had retreated up my forehead to such a degree that I looked like Mickey Mouse. No matter how warmly one holds Walt Disney’s friendy rodent, his appearance is seldom associated with young, ambitious go-getters.

As my twenties rolled by, so my hair and masculinity receded. It became increasingly hard to cover my balding forehead – there is only so much a swooping fringe can conceal. Then, in April 2016, just months before my wedding, aged 28, I finally took action. Vowing that my scalp would not take centre stage on my big day, I followed the lead of James Nesbitt, Wayne Rooney and thousands of others before me, and had hair restoration surgery.
I am not a slave to celebrity trends but it was undeniable: these men had seen results. Cold Feet star Nesbitt, 52, underwent several procedures very publicly and without embarrassment, which I found encouraging. Indeed, the actor has said that his hair transplants have given him a new lease of confidence and helped him win better roles.

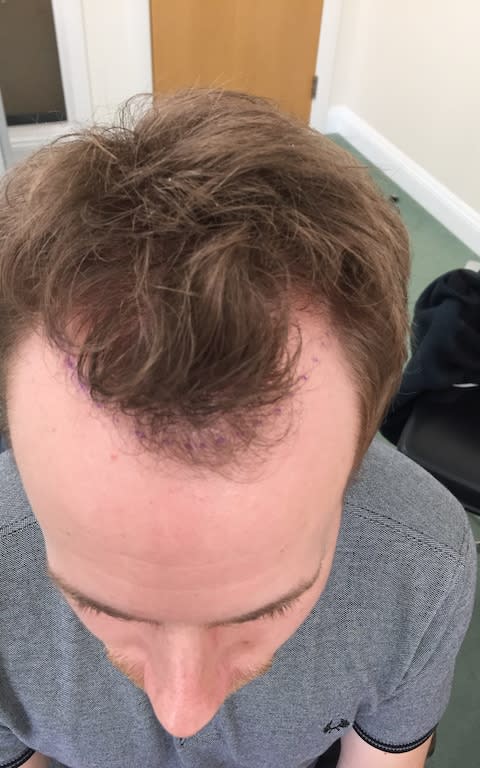
Today, two procedures at the Harley Street Hair Clinic that presided over Rooney’s well-publicised 2011 transplant, £10,000 in cash and a stress-free wedding later, I am invigorated. After two days of follicular unit extraction (FUE) – in which 1,200 tiny grafts were removed from the back of my head and rehomed up front – and a further round of scalp micro-pigmentation (SMP) to provide an extra illusion of thickness, these days I barely think about my hair. Where once I couldn’t catch my reflection without feeling dejected, now I feel brand new.
Yes, it sounds vain, but it is important to remember that hair loss can be more than a cosmetic issue. Just ask the 45 per cent of men who suffer male pattern baldness before 35. It can spark depression, body dysmorphic disorder, conditions such a trichotillomania, whereby the loss is worsened by repeated pulling out or twisting of the hair. Many find themselves withdrawing from daily life.
“I became a recluse,” says Spencer Stevenson, 41. “I was a confident, good-looking guy, had girlfriends and loved life. But when hair loss hit in my early twenties I was devastated.”

Stevenson invested more than £40,000 in restoring his hair, and now spends his time offering advice via his website (spexhair.com), or at in-person consultations. “I’ve had 10 hair transplants but I made so many mistakes and had nobody to speak to. For me, it has became a mission to help people.”
It is a patchy landscape for men to navigate. As Stevenson explains to his clients, catch hair loss quick enough and surgery might be avoided. However, with the hair restoration industry ringing up £2 billion of sales a year, the market is crammed with bogus remedies.
The handful of products that are proven by science to fight baldness include hair stimulant minoxidil (sold in the UK as Regaine) and Nizoral, an anti-dandruff shampoo shown to be effective against alopecia. The gold standard, however, is finasteride (marketed as Propecia), which hit headlines this month after US President Donald Trump was outed as a user by his long-time doctor.
First developed as a prostate drug, and plagued by claims that it lowers the sex drive, it is nonetheless hailed as a “miracle” among sufferers and surgeons alike. Dr Edward Ball, 41, owner of London’s Maitland Clinic explains that it works by blocking the conversion of testosterone into dihydrotestosterone (DHT), the thing that attacks the hair follicle, and can slow hair loss, or even stop it altogether. “Finasteride is the single best treatment available,” he says. “I talk about it as being like a miracle drug, because it really is. It works incredibly well, and only two to three per cent experience side effects.”
Despite continued leaps in technology, the surgery market around baldness can still embody the Wild West. Of Stevenson’s 10 procedures, most were attempts to fix the first “unnatural, pluggy” transplant he had in 2000. Dr Ball notes that unlicenced bargain clinics are “popping up” all over the world, while admitting that even he was seduced by the latest innovation when going under the knife in 2011.
The Artas robotic hair transplant system is a machine that aims to combine the skill of a surgeon with the precision and speed of technology. Simply, it moves around the head and quickly removes the hundreds of grafts needed to carry out FUE, rather than a surgeon doing so by hand. It was first used in Britain in 2013, but Dr Ball was a guinea pig.
“I started losing hair in my twenties and it became very thin on top,” he says. “I was working in a clinic in Los Angeles when we got the first Artas machine, so I was the research baby. They wanted me to speak very highly of the robot, but I can’t do that – it wasn’t fantastic.”
He worries that patients signing up to robotic transplant might be dazzled by the technology, instead of opting for the course of action that is right for them.
“There’s never going to be one treatment that suits everyone, because we are all different, from scalp texture to the shape of the head.
“That’s what I find frightening – even as a doctor, I still made the decision that this one solution was the best, because it was new and high tech. Of course, new things aren’t necessarily the best. My next procedure will be done manually, not by a robot.”
One thing is clear: research is key. “There are only a handful of top surgeons in the world that I would trust my head with,” agrees Stevenson.
The main consideration is the availability of donor hair, which is found at the back of the patient’s head. This is immune to baldness but once harvested does not grow back, meaning the supply is limited. It is crucial that the grafts are taken out carefully and don’t leave visible space or thinning - done wrong, you’re left with the dual pain of a poor transplant and fewer grafts to work with next time. A legitimate surgeon will match each patient to the transplant method best suited to them, as they may only have one shot at success.
This may mean eschewing FUE, the procedure de jour, in favour of follicular unit transplantation (FUT). Also known as the strip method, FUT removes a small portion of tissue from the back of the head and transplants it to where the patient is balding. It harvests from a wider supply of hair than FUE, but leaves behind an unavoidable scar. When performed by a seasoned professional, Dr. Ball claims this will be a mere “pencil line”. Done badly, Stevenson says it can look more like a “shark bite”.

Of course, such dilemmas may soon be rendered irrelevant, should pioneering research bear fruit. Discussions around 3D printed follicles, cell transplants and hair cloning abound. But although Dr. Ball believes a hair revolution may come, in the short term he advises caution.
“There is a lot of investment going into what’s considered the holy grail of hair restoration - an unlimited donor supply of hair, or even reversing hair loss without the need for surgery.
“The big thing to be careful of is saying, 'In five years we’ll have this breakthrough’, because that’s been said for 20 years,” he says.
But there remains hope.
“I sometimes feel depressed that the career I love may one day be taken away from me,” adds Dr Ball, “but it’s exciting to think we have an opportunity to to end hair loss."
“I look at my young son and think 'You’re going to lose hair because I do’. But I’m very hopeful there will be some serious treatment options that could provide baldness cures in his lifetime.”


